Translational Perioperative and Pain Medicine (ISSN: 2330-4871)
ARTICLE DOI: 10.31480/2330-4871/068
RESEARCH ARTICLE OPEN ACCESS
An ICU Preanesthesia Evaluation Form Reduces Missing Preoperative Key Information
Katherine Chuy1, Zhe Yan2, Lee Fleisher1 and Renyu Liu1
1Department of Anesthesiology and Critical Care, Perelman School of Medicine, University of Pennsylvania, USA
2Visiting Anesthesiologist, Department of Anesthesiology, First People's Hospital of Foshan, University of Pennsylvania, Guangdong, China
Renyu Liu, MD, PhD, Assistant Professor, Department of Anesthesiology and Critical Care, Perelman School of Medicine, University of Pennsylvania, 3620 Hamilton Walk, 336 John Morgan Building, Philadelphia, PA 19104, USA, Tel: 2156623750, Fax: 2153495078, E-mail: liur@uphs.upenn.edu
Editor: Daqing Ma, MD, PhD, FRCA, Professor of Anaesthesia and BOC Chair, Head of Anaesthesia Research, Imperial College London, G3, 44 Chelsea & Westminster Hospital, 369 Fulham Road, London SW10 9NH.
Received: February 02, 2018 | Accepted: March 28, 2018| Republished: April 06, 2018
Citation: Chuy K, Yan Z, Fleisher L, Liu R. An ICU Preanesthesia Evaluation Form Reduces Missing Preoperative Key Information. Transl Perioper & Pain Med 2018; 5 (2):40-48.
Abstract
Background
A comprehensive preoperative evaluation is critical for providing anesthetic care for patients from the intensive care unit (ICU). There has been no preoperative evaluation form specific for ICU patients that allows for a rapid and focused evaluation by anesthesia providers, including junior residents. In this study, a specific preoperative form was designed for ICU patients and evaluated to allow residents to perform the most relevant and important preoperative evaluations efficiently.
Methods
The following steps were utilized for developing the preoperative evaluation form: 1) Designed a new preoperative form specific for ICU patients; 2) Had the form reviewed by attending physicians and residents, followed by multiple revisions; 3) Conducted test releases and revisions; 4) Released the final version and conducted a survey; 5) Compared data collection from new ICU form with that from a previously used generic form. Each piece of information on the forms was assigned a score, and the score for the total missing information was determined. The score for each form was presented as mean ± standard deviation (SD), and compared by unpaired t test. A P value < 0.05 was considered statistically significant.
Results
Of 52 anesthesiologists (19 attending physicians, 33 residents) responding to the survey, 90% preferred the final new form; and 56% thought the new form would reduce perioperative risk for ICU patients. Forty percent were unsure whether the form would reduce perioperative risk. Over a three month period, we randomly collected 32 generic forms and 25 new forms. The average score for missing data was 23 ± 10 for the generic form and 8 ± 4 for the new form (P = 2.58E-11).
Conclusions
A preoperative evaluation form designed specifically for ICU patients is well accepted by anesthesia providers and helped to reduce missing key preoperative information. Such an approach is important for perioperative patient safety.
Keywords
Intensive care unit, Operating room, Anesthesia, Patients
Introduction
Patients in the intensive care unit (ICU) represent the sickest, least stable patients in the hospital setting. Many require infusions of vasoactive drugs, various complex forms of mechanical ventilation, or heart-support devices. It is not uncommon for these patients to undergo surgery as a last minute "add on" or emergency case. In many instances, a patient may arrive in the operating room (OR) from the ICU before anesthesia providers have an opportunity to perform a comprehensive preoperative evaluation. Acute hypoxemia and severe hemodynamic instability are not uncommon upon patient arrival in the OR due to inadequate preoperative preparation which may result in cancelling the case and returning the patient to the ICU or proceeding with the case with a high probability of a poor outcome [1]. An ICU patient's condition can change rapidly. The frequency with which new medical events occur, laboratory or imaging test results are updated, and infusions orders are changed necessitates a method for obtaining the most updated information on each patient before entering the OR. Current preoperative assessment systems not specifically designed for the ICU patient may not reflect these changes in a timely and concise manner. To reduce these potential gaps in information, it is critical to create a system or checklist that will allow focused and timely evaluations of ICU patients, improve communication of critical information between care providers, and provide for optimal preparation before the patient arrives in the OR.
Currently, there is no universal generic form for preoperative anesthesia evaluations. Furthermore, there is no preoperative evaluation form, either in electronic or paper format, specific for ICU patients in our institution. While ICU paper charts, online database system, and bedside evaluations provide most relevant information about an ICU patient's current status, such as a patient's ventilation mode and status or current vasopressor requirements, substantial time may be needed to fully understand a current patient's medical status and prepare a safe anesthetic plan. Residents performing this evaluation may overlook information in the process or forget to write it down, especially when transferring this information to a generic form that does not specifically ask for this information. In this study, we hypothesize that utilizing a well-designed preoperative form specifically designed for ICU patients would be accepted by anesthesia providers and reduce the incidence of missing key preoperative information.
Methods
The study was approved by the Institutional Review Board of the University of Pennsylvania Perelman School of Medicine. Our design of a new ICU preoperative evaluation form was based on a generic preoperative form (Figure 1, left panel) used at the Hospital of the University of Pennsylvania (HUP) for many years. The generic form was previously used to assess all patients preoperatively, whether they were ambulatory surgery patients, same day admissions, medical floor inpatients, or ICU patients. All headings on the generic form were included in the new ICU form to maintain familiarity and comprehension. We then added information that was deemed important for the perioperative evaluation of an ICU patient, such as specific ventilation modes and settings, intravascular lines and access, and current antibiotic regimens. The new ICU form (Figure 1, right panel) was subjected to multiple test releases and revisions in 2010; revisions were based on small group discussions and feedback from attending physicians and residents. Each test release occurred over a 1-month period, followed by subsequent revisions based on feedback. The version used in this study (Figure 1, right panel) was used over a 2-month period, followed by a formal evaluation comparing the two forms. An online anonymous survey was performed using survey monkey (http://www.surveymonkey.com/). The key questions asked in the survey were as follows: 1) Do you prefer this new form as compared to the old general preop form? 2) Do you think this form will reduce ICU patient risk perioperatively? 3) Are you a resident or attending? 4) Any comment or critics or suggestions? This questionnaire was used to assess feedback for the new form before data collection started for the study. The survey was created so that only one submission from one computer was allowed. Thus, each submission represents a unique answer. Anesthesiologists completing the survey were not aware of a future study comparing the two forms.
Figure 1: Generic and new ICU preoperative form. Generic preoperative form (left): Evaluation form used by anesthesia residents for preoperative data collection. Before creation of the new ICU preoperative form, this form was used for the evaluation of all patients, including non-ICU and ICU patients, prior to surgery. Currently, this is the form used to evaluate outpatients and inpatients not requiring critical care needs prior to surgery. New ICU preoperative form (right): New evaluation form created for preoperative data collection for ICU patients prior to surgery. The overall format from the generic preoperative form was maintained to optimize familiarity and comprehension of the new form. Headings deemed important for perioperative evaluation of an ICU patient were added to facilitate more comprehensive data collection. These include specific ventilation modes and settings, intravascular lines and access, and antibiotic regimens. The ICU form was finalized after multiple test releases and revisions.

We assessed written preoperative evaluation forms completed by anesthesia residents during a three month period. Forms were manually completed by first- through third-year anesthesia residents. Included in this study were those evaluations completed for surgical, medical, cardiac, or neurosurgical ICU patients undergoing either elective or emergency non-cardiac operations in the operating rooms at HUP. Both the generic and new forms were available for use, and residents selected the form of their own choice. Residents completing these evaluations were unaware of the ongoing study. Completed forms were collected randomly and evaluated.
A subjective scoring system for the key elements that may affect the anesthetic plan and perioperative care was created using a Delphi method (Table 1). Each piece of information was assigned a score based on its importance, with higher scores assigned to information with higher importance. Missing information received a value; higher scores for a specific preoperative evaluation reflected more missing information. Data are presented as mean ± standard deviation (SD). Data for each form were compared with an unpaired t test or Fisher exact test when appropriate. P value < 0.05 was considered statistically significant.
Table 1: Table of information tracked on evaluation forms and points assigned to each key piece of information. Higher scores were assigned to information considered to be more important. Missing information received a score value; higher scores for a specific preoperative evaluation reflected more missing information.
| Points | ||
| Patient body habit | 4 | |
| Height | 2 | |
| Weight | 2 | |
| Airway evaluation | 10 | |
| Current status | 5 | |
| H/o Airway management | 5 | |
| Vent settings | 10 | |
| Mode | 2 | |
| PEEP | 2 | |
| FiO2 | 2 | |
| Other settings | 2 | |
| Vent switch - allowed? | 2 | |
| Current vitals | 6 | |
| SpO2 | 2 | |
| BP | 2 | |
| HR | 2 | |
| Special monitoring | 5 | |
| Lines/Access | 5 | |
| Anesthesia history | 2 | |
| History | 1 | |
| Record if history present | 1 | |
| Eneteral feeds - cont/on hold/NPO | 1 | |
| Allergies (inc. Latex allergy) | 5 | |
| Labs | 6 | |
| HB | 2 | |
| K | 2 | |
| Cr | 2 | |
| Blood availability | 10 | |
| Preop T&S | 5 | |
| Preop T&C | 4 | |
| Blood antibodies? | 1 | |
| PMH | 5 | |
| Past surgical history | 2 | |
| Medications | 10 | |
| Anti-coagulations | 2 | |
| Infusions (Pressors and Others) | 2 | |
| Antibiotic regimen (last dose, next dose) | 2 | |
| Antibiotic regiment - last dose | 2 | |
| Antibiotic regiment - last dose | 2 | |
| Last dialysis if applicable | 5 | |
| Studies - ECHO etc | 5 | |
| Information of the scheduled procedure | 1 | |
| Anesthesia consent | 5 | |
| Anesthesia Plan | 4 | |
| Total | 100 |
Results
The results from the survey
Out of a total of 85 attending and 72 first- through third-year anesthesia residents anesthesiologists, 52 anesthesiologists (19 attending physicians and 33 first- through third-year anesthesia residents) responded to the online survey, corresponding to an overall response rate of 39%. Out of the residents who responded to the survey, 15 were first year anesthesia residents (46%), 10 were second year anesthesia residents (30%), and 8 were third year anesthesia residents (24%). Out of all anesthesiologists who responded, the survey indicated that 90% (47 out of 52) preferred the new form, and 56% (28 out of 50) thought the new form would reduce perioperative risk for ICU patients. Forty percent were unsure whether the form would reduce perioperative risk. Given that the form was well received, it is now the official preoperative form for ICU patients undergoing surgery approved by the institutional form committee as indicated in Figure 2. The specific anesthetic planning items were added into the currently released form since anesthetic plan is one of the missing data in the previous versions.
Figure 2: The currently implanted preoperative evaluation form for the ICU patients for surgery.

Some comments from the survey included: "Very easy to read and gather information quickly. All the important information is highlighted included airway/pressors and lines. For very sick patients, this is a much better form"; "Well organized and all the pertinent information is there"; "A very thorough form"; "Love the new form"; "This form looks great" and "Having all the information in one place is (great)".
Examples of suggestions from the survey include: "You may need two pages, or perhaps add an optional basically blank second page. Not everyone is suitable for one page form. Past medical history should include ICU events that may need an optional second page that is devoid of check marks and fillings"; "I think it would be better for the resident doing the pre-op to simply fill in relevant info (without the template). This would give the resident a chance to actually think about the case and what patient info is most (important)".
Comparison of missing data
Over three month period, we randomly collected 32 generic forms and 25 new forms. The average score for missing data was 23 ± 10 for the generic form and 8 ± 4 for the new form (P < 0.0001).
Thirteen of 32 generic preoperative forms lacked information regarding ventilation mode or airway status, whereas only two out of 25 new preoperative forms lacked such information (P = 0.0066). Other missing data in both of the forms are presented in Figure 3. There are significant overlaps in some areas of missing data.
Figure 3: The comparison of missing information in generic versus new ICU preoperative form. X axis is the score of the missing information. The higher score indicates more missing key information. Y axis is the type of missing information. It is apparent that higher score in most of the categories of the missing information. Some overlap of the missing information in both of the forms is also noted.
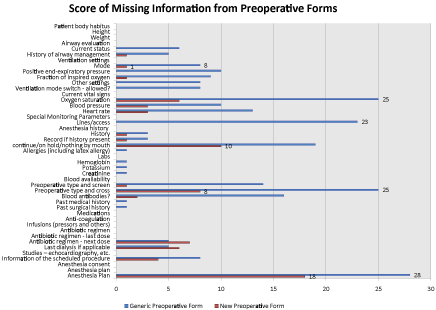
Of note, the most common missing information in the generic form was the type of anesthetic and procedures consented for (anesthesia plan) (28 out of 32), current oxygen saturation (25 out of 32), preoperative type and cross/match status (26 out of 32), and lines/access (23 out of 32) (Figure 2). For the new form, the most common missing information was anesthesia plan (18 out of 25), enteral feed status (10 out of 25), and preoperative type and cross status (8 out of 25).
Discussion
Our study demonstrates that a structured preoperative evaluation form specifically designed for the ICU patient is well accepted by anesthesia providers in a large academic institution and reduces missing key preoperative information.
Why an ICU preoperative form is needed?
The importance of a comprehensive preoperative evaluation cannot be understated since it forms the basis for an optimal anesthetic plan [2-4]. This is crucial for the perioperative care of ICU patients because they are at increased risk for morbidity and mortality relative to outpatients and other inpatients not requiring critical care [5-7]. Furthermore, emergency surgery increases mortality risk up to 10-fold compared to elective surgery, particularly in patients with ASA grade 4 or 5 [7,8]. Emergent cases in critically ill patients frequently result in limited time and opportunity for a careful preoperative evaluation resulting in missing key information for an optimal anesthetic plan.
The preoperative evaluation for ICU patients often entails more details than that for patients presenting from home or the ward. This is especially true regarding the history of anesthesia, current vital signs, specific lines and access, ventilation settings, airway status, and particular pulmonary and cardiac comorbidities. With the new ICU form, these items are all available in a one-page format. This provides anesthesiologists comprehensive information about a patient in an efficient manner, saving time and allowing the anesthesiologist to focus on creating an anesthesia plan to reduce potential perioperative risks for ICU patients. If needed, copies of test reports from echocardiograms or stress tests and of records from a previous anesthetic can be provided with the form as additional reference information. The ability to maintain a high level of comprehensive information in the transition of care of critically ill patients is crucial to the safety and adequacy of anesthesia care, particularly when an emergent case is scheduled and limited time is available to prepare for the patient [9]. Implementation of this form might help in the transition of care amongst resident trainees in the perioperative evaluation of ICU patients.
While a board-certified anesthesiologist may not require a template to properly assess ICU patients for surgery, a well-designed preoperative evaluation form is helpful for training new anesthesia providers on collecting important information to consider when assessing ICU patients prior to surgery. With this preoperative form, junior anesthesia providers would be guided to collect certain critical information essential in creating an optimal anesthesia plan and preparing for any specific anesthetic considerations. Thus, a well organized preoperative form helps new anesthesia providers develop an organized way of assessing ICU patient's perioperatively with detail and efficiency.
Our results showed that use of the new ICU preoperative evaluation form resulted in significantly less missing data compared to the generic form. Whereas there was some overlap in the type of information missing from both forms, certain information considered important was present significantly more frequently on the new form, such as current vital signs and specific lines/access. The ability to capture this data with the new ICU form allows the anesthesiologists to adequately prepare for specific monitoring. For example, preparation for arterial blood pressure, central venous pressure, or pulmonary artery pressure monitoring, or knowing that the patient has limited intravenous access, can allow the anesthesiologist to prepare the proper OR monitoring devices and make appropriate judgments regarding the placement of additional intravenous lines.
Of particular note is that information regarding ventilation a setting was lacking significantly more often from the completed generic forms compared to the completed new forms. Ventilation settings are extremely important for the anesthesiologist, particularly if that patient has a specific physiologic status that prevents him/her from obtaining adequate ventilation on conventional ventilation settings by the operating room anesthetic machine and therefore may require bringing an ICU ventilator to the OR. In addition, completed generic forms frequently lacked information regarding previous airway management compared to completed new forms. This is also particularly important because certain information can help identify potential difficult anesthetic issues [10]. For example, information about a history of a difficult airway, limited cervical extension, presence of a neck collar or brace, halo, or a large amount of soft tissue surrounding the neck, would likely lead the anesthesiologist to alter the airway management plan.
Because the ICU form demonstrates a decrease in the number of missing critical data and aids in the transfer of information among anesthesia providers, it theoretically should reduce perioperative risk in ICU patients. However, further studies are needed to assess this potential risk reduction. We would need a much larger sample size and would need to outline data points to follow regarding risk reduction and any benefits to anesthetic planning. Future evaluation of the ICU form may benefit from asking anesthesia providers if the form meets their needs for the case and if they require any additional data.
Key components of the ICU preoperative evaluation form
Essential data for proper evaluation includes past medical history, social history (use of tobacco, alcohol, drugs), allergies, current and recent drug therapy, problems or complications associated with previous anesthetics, family history of adverse reactions to anesthesia, vital signs, as well as results of important laboratory tests, electrocardiograms, and chest radiograms, if warranted [6,11,12].
Compared to the generic preoperative assessment form, the new form requires that information specific to an ICU patient be completed before handoff to individuals providing anesthetic care in the OR. Including key components specific to ICU patients likely aided in its acceptance among anesthesia providers and continued success. These key components include history of airway management; ventilation settings; current vital signs, tube feed status; special monitoring parameters; lines and access; the presence of an anesthesia history in our electronic health record system; blood availability; various infusions; antibiotic regimens including the last and next scheduled dose times; last dialysis if applicable; and specific anesthesia consents and plans.
This information allows residents to efficiently devise an anesthesia plan with the attending physician when time is limited. With a known antibiotic regimen, the resident can prepare for appropriate intraoperative antibiotic dosing by preparing dilutions or obtaining medications from the pharmacy. Information regarding specific ventilation settings allows residents to communicate with respiratory therapists and anticipate intraoperative airway management and respiratory care, particularly for patients with complicated pulmonary issues requiring unique ventilation mode not regularly available in ORs. In addition, information regarding central lines, pulmonary artery pressure monitoring and intracranial pressure monitoring, will allow preparation for monitors and anticipate their usage.
Transition into an electronic form
While this form is designed on a paper format, it could and should serve as the foundation for a computerized preanesthesia evaluation form for ICU patients, contributing to a patient's electronic medical record (EMR). It would be ideal if all these information could be populated with the real-time database in the EMR. While electronic preanesthesia record has been on the market for a relatively long time, we are unaware of an electronic preanesthesia record that reflects the characteristic information for ICU patients: The complexity and severity of current illness, fast changing condition with special ventilation settings and cardiovascular supporting agents. The incompatibility of an electronic record system in the ICU with the electronic record system in the OR is another hurdle to have an electronic preanesthesia evaluation. Thus, the paper preanesthesia evaluation form may continue to be required until such an electronic record could be developed. However, it is important to input collected preoperative information into the electronic record during the case for record keeping and data mining for outcome studies in the future.
Limitations, critiques and future directions
Although the ICU preoperative evaluation form has been formally adopted, further revisions may be needed. For example, tracheostomy is not listed as one of the airway management regimens and this would be useful information to know prior to surgery. Some anesthesia providers suggest that it is meaningless to list the goals of fluid inputs and outputs. While many anesthesia providers think that this ICU specific preoperative evaluation form might reduce perioperative risk and improve outcome, well-designed prospective studies are warranted to study this. Of note, 90% of anesthesia providers completing the initial survey reported preferred the new ICU form in evaluating critically ill patients. During the data collection period, however, more residents chose the general form to complete their evaluations for ICU patients. This may reflect the familiarity residents had with the general form, as they had been using it regularly for preoperative assessments of ICU patients or the ease of its use compared to the more complicated form. Future studies would benefit from performing a randomized trial of the two forms. In addition, the number of different residents and correlation between residency classes and completeness of the forms was not followed. However, all anesthesia residents perform preoperative evaluations for ICU patients without regard to level of training. Future studies would benefit from specifically noting the level of training of resident completing the form.
In summary, we designed and evaluated the effectiveness of a new preoperative anesthesia evaluation form specifically structured for ICU patients and compared it to a generic unstructured form with respect to comprehensive data collection. The new form resulted in reduced missing information. Also, the new form was well accepted by anesthesia providers and is currently an official preanesthesia evaluation form approved by the institutional form committee for ICU patients prior to surgery. Further studies will determine whether use of this form reduces perioperative risk in these patients by ensuring adequate information transfer from different locations of care.
Acknowledgement
The authors thank Mrs. Mary S. Hammond for obtaining IRB approval.
Disclosure of Funding
This research was supported by departmental funding from the Department of Anesthesiology and Critical Care at the University of Pennsylvania and NIH K08-GM-093115-01(PI:RL).
Institution
Perelman School of Medicine at the University of Pennsylvania and Emory University School of Medicine.
References
- Lau HK, Chen TH, Liou CM, Chou MC, Hung WT (2010) Retrospective analysis of surgery postponed or cancelled in the operating room. J Clin Anesth 22: 237-240.
- Zambouri A (2007) Preoperative evaluation and preparation for anesthesia and surgery. Hippokratia 11:13-21.
- Davies SJ, Wilson RJ (2004) Preoperative optimization of the high-risk surgical patient. Br J Anaesth 93: 121-128.
- Girbes AR (2000) The high-risk surgical patient and the role of preoperative management. Neth J Med 57: 98-105.
- Cohen MM, Duncan PG, Tate RB (1988) Does anesthesia contribute to operative mortality? JAMA 260: 2859-2863.
- Myers ML (1998) Preoperative Evaluation Jacksonville Medicine. Jacksonville.
- Asouhidou I, Asteri T, Sountoulides P, Natsis K, Georgiadis G (2009) Early postoperative mortality in the elderly: a pilot study. BMC Res Notes 2:118.
- Leung JM, Dzankic S (2001) Relative importance of preoperative health status versus intraoperative factors in predicting postoperative adverse outcomes in geriatric surgical patients. J Am Geriatr Soc 49:1080-1085.
- Arora V, Johnson J (2006) A model for building a standardized hand-off protocol. Jt Comm J Qual Patient Saf 32:646-655.
- Garcia-Miguel FJ, Serrano-Aguilar PG, Lopez-Bastida J (2003) Preoperative assessment. Lancet 362:1749-1757.
- Sigworth SK (2008) Preoperative evaluation of hospitalized patients. Mt Sinai J Med 75: 442-448.
- Fitz-Henry J (2011) The ASA classification and peri-operative risk. Ann R Coll Surg Engl 93:185-187.